Institute for Response-Genetics (e.V.)Chairman: Prof. Dr. Hans H. StassenPsychiatric Hospital (KPPP), University of Zurich |

|


|
Polypharmacy in PsychiatryCurrent treatment standards in psychiatry are oriented towards polypharmacy, that is, patients receive combinations of several antidepressants, antipsychotics, mood stabilizers, anxiolytics, hypnotics, antihistamines, and anticholinergics, along with other somatic treatments. In tandem with the beneficial effects of psychopharmacological drug treatment, patients experience significant adverse reactions which appear to have become more frequent and more severe with the rise of ubiquitous polypharmacy. Clinical Study of 320 PatientsIn a longitudinal study of 320 patients, we assessed today's acute inpatient treatment of depressive (ICD10 F3) and schizophrenic (ICD10 F2) disorders with focus on therapeutic strategies, medications, adverse side effects, time course of recovery, and efficacy of treatments. Of particular interest was the weighing of the benefits and drawbacks of polypharmacy regimens. Polypharmacy was by far the most common treatment regimen (85%). On average, patients received 4.50 ± 2.68 medications, consisting of 3.30 ± 1.84 psychotropic drugs, plus 0.79 ± 1.13 medications that alleviate adverse side effects, plus 0.41 ± 0.89 other somatic medications. The treating psychiatrists appeared to be the main determining factor in this context, while «previous history» and «severity at baseline» played a minor role, if at all. Adverse Drug ReactionsAdverse drug reactions were found to be an inherent component of polypharmacy and tended to have a 2-3 times higher incidence compared to monotherapy. Severe adverse reactions could not be attributed to a particular drug or drug combination. Rather, the empirical data suggested that severe side effects can be triggered by virtually all combinations of drugs, provided patients have a respective vulnerability. In terms of efficacy, there were no advantages of polypharmacy over monotherapy. RecommendationsPolypharmacy regimens are not equally suited for every patient. Specifically, such regimens appear to have a negative impact on treatment outcome and to obfuscate the «natural» time course of recovery through a multitude of interfering factors. Evidence clearly speaks against starting just every therapeutic intervention in psychiatry with a combination of psychopharmaceuticals. We think that it is time for psychiatry to reconsider its treatment strategies, which are far too one-sidedly fixated on psychopharmacology and pay far too little attention to alternative approaches, especially in mild cases where psychotherapy without concurrent medication should still be an option. Also, regular exercises and sports can definitely be an effective therapeutic means in a considerable number of cases. General practitioners (GPs) are particularly in demand here [Stassen et al. 2021]. References
Stassen HH, Bachmann S, Bridler R, Cattapan K, Hartmann AM, Rujescu D, Seifritz E. Genetic
Predisposition to Unwanted Side Effects under Antidepressants and Antipsychotics: A
molecular-genetic study of 902 patients over 6 weeks. Eur Arch Psychiatry Clin Neurosci.
2026; 276(2): 691-707. doi: 10.1007/s00406-025-02062-4. Epub 2025 Jul 28.
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Seifritz E. Polypharmacy in Psychiatry and
Weight Gain: Longitudinal Study of 832 Patients Hospitalized for Depression or Schizophrenia,
along with Data of 3,180 Students from Europe, the U.S., South America, and China.
Eur Arch Psychiatry Clin Neurosci. 2025; 275(4): 1001-1014. doi: 10.1007/s00406-024-01767-2.
Epub 2024 Mar 10.
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Hartmann AM, Rujescu D, Seifritz E, Weisbrod M,
Scharfetter C: Genetic Determinants of Antidepressant and Antipsychotic Drug Response:
A molecular-genetic study of 902 patients over 6 weeks. Eur Arch Psychiatry Clin Neurosci. 2025;
275(5): 1419-1435. doi: 10.1007/s00406-024-01918-5. Epub 2024 Oct 9.
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Hartmann AM, Rujescu D, Seifritz E, Weisbrod M,
Scharfetter C. Analysis of genetic diversity in patients with major psychiatric disorders
versus healthy controls: A molecular-genetic study of 1698 subjects genotyped for 100 candidate
genes (549 SNPs). Psychiatry Res. 2024; 333: 115720. doi: 10.1016/j.psychres.2024.115720
[get the article]
Greil W, de Bardeci M, Müller-Oerlinghausen B, Nievergelt N, Stassen HH, Hasler G, Erfurth A,
Cattapan K, Rüther E, Seifert J, Toto S, Bleich S, Schoretsanitis G. Controversies regarding
lithium-associated weight gain: case-control study of real-world drug safety data.
Int J Bipolar Disord. 2023; 11(1): 34. doi: 10.1186/s40345-023-00313-8
[get the article]
de Bardeci M, Greil W, Stassen H, Willms J, Köberle U, Bridler R, Hasler G, Kasper S, Rüther E,
Bleich S, Toto S, Grohmann R, Seifert J. Dear Doctor Letters regarding citalopram and escitalopram:
guidelines vs real-world data. Eur Arch Psychiatry Clin Neurosci. 2023; 273(1): 65-74
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Herzig D, Schneeberger A, Seifritz E:
Detailing the Effects of Polypharmacy in Psychiatry: Longitudinal Study of 320 Patients
Hospitalized for Depression or Schizophrenia. Eur Arch Psychiatry Clin Neurosci. 2022;
272(4): 603-619
[get the article]
Moragrega I, Bridler R, Mohr C, Possenti M, Rochat D, Sanchez Parramon J, Stassen HH:
Monitoring Mental Health and the Effects of Therapeutic Interventions through Self-Assessment
Voice Analyses. Res Psychother. 2021, 24(3): 250-262
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Herzig D, Schneeberger A, Seifritz E. Inflammatory
Processes linked to Major Depression and Schizophrenic Disorders and the Effects of Polypharmacy
in Psychiatry: Evidence from a longitudinal Study of 279 Patients under Therapy. Eur Arch
Psychiatry Clin Neurosci. 2021; 271(3): 507-520
[get the article]
Greil W, de Bardeci M, Seifert J, Bernegger X, Cattapan K, Stassen HH, Wagner AL, Sieberer M,
Grohmann R, Toto S: Treatment of depression: Are psychotropic drugs appropriately dosed in women
and in the elderly? Dosages of psychotropic drugs by sex and age in routine clinical practice.
Hum Psychopharmacol. 2022; 37(1): e2809
[get the article]
Pollak TA, Lennox B, Müller S, Benros ME, Prüss H, Tebartz van Elst L, Klein H, Steiner J, Frodl T,
Bogerts B, Tian L, Groc L, Hasan A, Baune BT, Endres D, Haroon E, Yolken R, Benedetti F, Halaris A,
Meyer J, Stassen H, Leboyer M, Fuchs D, Otto M, Brown DA, Vincent A, Najjar S, Bechter K: An
international consensus on an approach to the diagnosis and management of psychosis of suspected
autoimmune origin: the concept of autoimmune psychosis. Lancet Psychiatry 2020; 7(1): 93-108
Zhang M, Bridler R, Mohr C, Moragrega I, Sun N, Xu Z, Yang Z, Possenti M, Stassen HH: Early
Detection of the Risk of Developing Psychiatric Disorders: A Study of 461 Chinese University
Students under Chronic Stress. Psychopathology 2019; 52(6): 367-377
[get the article]
Bhake R, Kluckner V, Stassen HH, Russell GM, Leendertz J, Stevens K, Linthorst ACE, Lightman S:
Continuous Free Cortisol Profiles — Circadian Rhythms in Healthy Men. J Clinical Endocrinology &
Metabolism 2019; 104(12): 5935-5947
Stassen HH, Bachmann S, Bridler R, Cattapan K, Herzig D, Höppner K, Schneeberger A, Seifritz E,
Wirth A, M. Weisbrod M: Polypharmacy in Psychiatry: Unwanted Side Effects and Inflammatory Response
System — A Naturalistic Study of 195 Patients under Treatment. Eur Neuropsychopharmacology 2019;
29 Suppl 1: S345
Greil W, Zhang X, Stassen HH, Grohmann R, Bridler R, Hasler G, Toto S, Bleich S, Kasper S: Cutaneous
adverse drug reactions to psychotropic drugs and their risk factors — a case-control study. Eur
Neuropsychopharmacol. 2019; 29(1): 111-121
[get the article]
Stassen HH: Heterogeneity of schizophrenic disorders and link to chronically elevated IgM values.
Neurology, psychiatry and brain research 2018; 29: 23-24
Stassen HH, Braun S, Bridler R, Seifritz E, Weisbrod M: Inflammatory Processes and Schizophrenia:
Evidence from a Twin Study. Eur Neuropsychopharmacology 2017; 27 Suppl 4: S934-S935
Braun S, Bridler R, Müller N, Schwarz MJ, Seifritz E, Weisbrod M, Zgraggen A, Stassen HH:
Inflammatory Processes and Schizophrenia: Two Independent Lines of Evidence from a Study
of Twins Discordant and Concordant for Schizophrenic Disorders. European Archives of
Psychiatry and Clinical Neuroscience 2017; 267: 377-389
[get the article]
Braun S, Annovazzi C, Botella C, Bridler B, Camussi E, Delfino JP, Mohr C, Moragrega I, Papagno C,
Pisoni A, Soler C, Seifritz E, Stassen HH: Assessing Chronic Stress, Coping Skills and Mood Disorders
through Speech Analysis. A Self-Assessment "Voice App" for Laptops, Tablets, and Smartphones.
Psychopathology 2016; 49(6): 406-419
[get the article]
Delfino JP, Barragán E, Botella C, Braun S, Bridler R, Camussi E, Chafrat V, Lott P, Mohr C,
Moragrega I, Papagno C, Sanchez S, Seifritz E, Soler C, Stassen HH: Quantifying Insufficient
Coping Behavior under Chronic Stress. A cross-cultural study of 1,303 students from Italy,
Spain, and Argentina. Psychopathology 2015; 48: 230-239
Mohr C, Braun S, Bridler R, Chmetz F, Delfino JP, Kluckner VJ, Lott P, Schrag Y, Seifritz E, Stassen HH:
Insufficient Coping Behavior under Chronic Stress and Vulnerability to Psychiatric Disorders.
Psychopathology 2014; 47: 235-243
Stassen HH, Delfino JP, Kluckner VJ, Lott P, Mohr C: Vulnerabilität und psychische Erkrankung. Swiss Archives
of Neurology and Psychiatry 2014; 165(5): 152-157
Giegling I, Balzarro B, Porcelli S, Schäfer M, Hartmann AM, Friedl M, Konte B, Krämer P, Möller HJ,
De Ronchi D, Stassen HH, Serretti A, Rujescu D: Influence of ANKK1 and DRD2 polymorphisms in
response to haloperidol. Eur Arch Psychiatry Clin Neurosci. 2013; 263(1): 65-74
Bridler R, Orosz A, Cattapan K, Stassen HH: In Need of Psychiatric Help - Leave a Message after
the Beep. Psychopathology. 2013; 46(3): 201-205
Drago A, Giegling I, Schäfer M, Hartmann AM, Friedl M, Konte B, Möller HJ, De Ronchi D, Stassen HH,
Serretti A, Rujescu D: AKAP13, CACNA1, GRIK4 and GRIA1 genetic variations may be associated with
haloperidol efficacy during acute treatment. Eur Neuropsychopharmacol. 2013; 23(8): 887-894
Drago A, Giegling I, Schäfer M, Hartmann AM, Möller HJ, De Ronchi D, Stassen HH, Serretti A,
Rujescu D: No association of a set of candidate genes on haloperidol side effects.
PLoS One. 2012; 7(10): e44853
Giegling I, Drago A, Dolzan V, Plesnicar BK, Schäfer M, Hartmann AM, Sander T, Toliat MR,
Möller HJ, Stassen HH, Rujescu D, Serretti A: Glutamatergic gene variants impact the clinical
profile of efficacy and side effects of haloperidol. Pharmacogenet Genomics. 2011; 21(4): 206-216
Kemp DE, Ganocy SJ, Brecher M, Carlson BX, Edwards S, Eudicone JM, Evoniuk G, Jansen W, Leon AC,
Minkwitz M, Pikalov A, Stassen HH, Szegedi A, Tohen M, Van Willigenburg AP, Calabrese JR: Clinical value
of early partial symptomatic improvement in the prediction of response and remission during short-term
treatment trials in 3369 subjects with bipolar I or II depression. J Affect Disord. 2011; 130(1-2): 171-179
Stassen HH, Anghelescu IG, Angst J, Böker H, Lötscher K, Rujescu D, Szegedi A, Scharfetter C:
Predicting Response to Psychopharmacological Treatment. Survey of Recent Results.
Pharmacopsychiatry 2011; 44: 263-272
Lötscher K, Anghelescu IG, Braun S, Bridler R, Stassen HH: Polypharmacy in psychiatry: clinical practice
versus empirical evidence. Eur Neuropsychopharmacol. 2010; 20 (Suppl. 3): 378-379
Szegedi A, Jansen WT, Van Willigenburg AP, Van der Meulen E, Stassen HH, Thase ME: Early
improvement as a predictor of treatment outcome in patients with major depressive disorder:
Why the first 2 weeks really matter - evidence from 6562 patients. J Clin Psychiatry 2009; 70(3): 344-353
Stassen HH, Angst J, Hell D, Scharfetter C, Szegedi A: Is there a common resilience mechanism
underlying antidepressant drug response? Evidence from 2848 patients. J Clin Psychiatry 2007;
68(8): 1195-1205
Stassen HH, Scharfetter C: Vulnerability, resilience and response to psychotropic drugs:
shared genetic factors? Am J Med Genetics 2006; 141: 707-708
Lavergne F, Berlin I, Gamma A, Stassen H, Angst J: Onset of improvement and response to
mirtazapine in depression: a multicenter naturalistic study of 4771 patients. Neuropsychiatric
Disease and Treatment 2005; 1(1): 59-68
Stassen HH, Angst J, Scharfetter C, Szegedi A: Therapie mit Antidepressiva: Erfolg von
genetischen Faktoren abhängig? Leading Opinions, Neurologie & Psychiatrie 2005; 6: 25-27
Stassen HH, Angst J: Wirkung und Wirkungseintritt in der Antidepressiva-Behandlung.
Medizinspektrum 2004; 15: 15-17
Stassen HH, Dahmen N, Hell D, Nürnberg P, Sander T, Toliat MR, Szegedi A: Genetic predisposition
of antidepressant drug response. Am J Med Genetics 2003; 122: 123-124
Montgomery SA, Bech P, Blier P, Moller HJ, Nierenberg AA, Pinder RM, Quitkin FM, Reimitz PE,
Rosenbaum JF, Rush AJ, Stassen HH, Thase ME: Selecting methodologies for the evaluation of
differences in time to response between antidepressants. J Clin Psychiatry 2002; 63(8):
694-699
Stassen HH, Angst J, Delini-Stula A: Fluoxetine versus moclobemide: cross-comparison between the
time course of improvement. Pharmacopsychiatry 1999; 32: 56-60
Stassen HH, Kuny S,. Hell D: The speech analysis approach to determining onset of improvement
under antidepressants. Eur Neuropsychopharmacology 1998; 8,4: 303-310
Stassen HH, Angst J, Delini-Stula A: Onset of improvement under fluoxetine and moclobemide.
Eur Psychiatry 1998; 13,3: 128-133
Angst J, Stassen HH: Methodische Probleme der Prüfung von Antidepressiva. In: Stieglitz RD,
Fähndrich E, Möller HJ (eds): Syndromale Diagnostik psychischer Störungen. Hogrefe, Göttingen
1998: 5-12
Stassen HH, Angst J, Delini-Stula A: Delayed onset of action of antidepressant drugs? Survey
of results of Zurich meta-analyses. Eur Psychiatry 1997; 12: 166-176
Stassen HH, Angst J, Delini-Stula A: Delayed onset of action of antidepressant drugs? Survey of
results of Zurich meta-analyses. Pharmacopsychiatry 1996; 29: 87-96
Kuny S, Stassen HH: Cognitive performance in patients recovering from depression. Psychopathology
1995; 28: 190-207
Stassen HH, Angst J: Methods of estimating onset of improvement. Eur Neuropsychopharmacology
1994; 4,3: 284-285
Stassen HH, Angst J, Delini-Stula A: Severity at baseline and onset of improvement in depression.
Meta-analysis of Imipramine and Moclobemide vs Placebo. Eur Psychiatry 1994; 9: 129-136
Stassen HH, Delini-Stula A, Angst J: Time course of improvement under antidepressant treatment:
a survival-analytical approach. Eur Neuropsychopharmacol 1993; 3: 127-135
Angst J, Delini-Stula A, Stabl M, Stassen HH: Is a cutoff score a suitable measure of
treatment outcome in short-term trials in depression? A methodological meta-analysis.
Human Psychopharmacology 1993; 8: 311-317
Angst J, Stassen HH, Woggon B: Effect of neuroleptics on positive and negative symptoms and
the deficit state. Psychopharmacology 1989; 99: 41-46
|
|
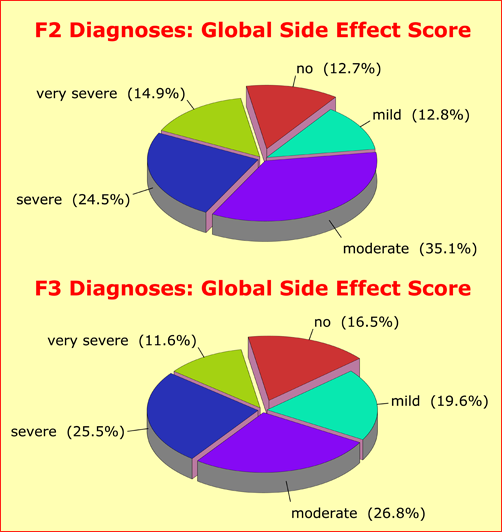
Most patients experience significant adverse side effects induced by their psychotropic medications. As many as 87.3% of the F2 patients reported at least «some» mild adverse effects, of which 39.4% were of severe or very severe form. The differences to F3 patients are marginal. |
|
| [ Mail to Webmaster ] k454910@ifrg.ch |