Institute for Response-Genetics (e.V.)Chairman: Prof. Dr. Hans H. StassenPsychiatric Hospital (KPPP), University of Zurich |

|


|
Incidence and LatencyThe two central aspects of psychotropic drug response, the proportion of patients in whom a therapeutic response is induced ("incidence") and the time to onset of improvement ("latency"), are often combined into a single, 1-dimensional "cure" model by means of survival-analytical techniques. This cure model incorporates non-responders in addition to modeling the time to an a priori defined clinical response. Patients who dropped out of the trial prior to the envisaged observation period are treated as "censored" data under the assumption of random censoring. The non-parametric generalized maximum likelihood for the model is obtained from the Kaplan-Meier (KM) product limit estimator. By contrast, when separating incidence and latency through a 2-dimensional cure model, tests become available [Kolmogorov-Smirnov, Cramer-von Mises] to explicitly compare the speed of improvement between treatments among improvers. Latency Explains No More than 5% of VarianceAmong patients who meet improvement or response criteria, the distribution of the individual onsets is slightly left-skewed, yet approximately normal, covering a wide range from early to late improvement/response with mean values around day 12-14 (improvement) and day 18-20 (response). Unexpectedly, there are almost no differences between treatment modalities in this respect, with differences between active compounds, and between active compounds and placebo, being reflected only by the total number of improvers and responders. The subtle differences in the "average" onset are likely the effect of non-standardized placebo washouts which may explain a ±2 day shift of baseline, or may relate to the dose titration differences in the first days of treatment. No Gender DifferencesAnalyses carried out separately for male and female patients did not reveal major gender differences, except for mirtazapine and paroxetine, where sample sizes were small. ⇒ Meeting improvement criteria is highly predictive of later outcome, as typically >70% of the patients who show sustained improvement within the first 10-14 days of treatment ("early improvement") later become sustained responders by the end of a typical six-week drug trial. Inversely, more than 80% of sustained responders at the end of a six-week drug trial show sustained improvement within the first 10-14 days of treatment, thus suggesting that in more than two thirds of the patients, the time course of improvement is sustained once the recovery has started. References
Agid O, Kapur S, Arenovich T, Zipursky RB. Delayed-onset hypothesis of antipsychotic
action: a hypothesis tested and rejected. Arch Gen Psychiatry 2003; 60(12): 1228-1235
Agid O, Seeman P, Kapur S. The "delayed onset" of antipsychotic action--an idea whose
time has come and gone. J Psychiatry Neurosci. 2006; 31(2): 93-100
Agid O, Kapur S, Warrington L, Loebel A, Siu C. Early onset of antipsychotic response
in the treatment of acutely agitated patients with psychotic disorders. Schizophr Res.
2008; 102(1-3): 241-248
Bhake R, Kluckner V, Stassen HH, Russell GM, Leendertz J, Stevens K, Linthorst ACE, Lightman S:
Continuous Free Cortisol Profiles – Circadian Rhythms in Healthy Men. J Clinical Endocrinology &
Metabolism 2019; 104(12): 5935-5947
Braun S, Bridler R, Müller N, Schwarz MJ, Seifritz E, Weisbrod M, Zgraggen A, Stassen HH:
Inflammatory Processes and Schizophrenia: Two Independent Lines of Evidence from a Study of Twins
Discordant and Concordant for Schizophrenic Disorders. Eur Arch Psychiatry Clin Neurosci 2017; 267: 377-389
[get the article]
Cassano P, Fava M. Tolerability issues during long-term treatment with antidepressants.
Ann Clin Psychiatry 2004; 16(1): 15-25
Chwastiak LA, Rosenheck RA, McEvoy JP, Keefe RS, Swartz MS, Lieberman JA.
Interrelationships of psychiatric symptom severity, medical comorbidity, and
functioning in schizophrenia. Psychiatr Serv. 2006; 57(8): 1102-1109
Correll CU, Malhotra AK. Pharmacogenetics of antipsychotic-induced weight gain.
Psychopharmacology 2004; 174(4): 477-489
Eaton WW, Byrne M, Ewald H, Mors O, Chen CY, Agerbo E, Mortensen PB. Association of
schizophrenia and autoimmune diseases: linkage of Danish national registers. Am J
Psychiatry 2006; 163(3): 521-528
Fleischhacker WW, Cetkovich-Bakmas M, De Hert M, Hennekens CH, Lambert M, Leucht S,
Maj M, McIntyre RS, Naber D, Newcomer JW, Olfson M, Osby U, Sartorius N, Lieberman JA.
Comorbid somatic illnesses in patients with severe mental disorders: clinical, policy,
and research challenges. J Clin Psychiatry. 2008;69(4): 514-519
Geddes J, Freemantle N, Harrison P, Bebbington P. Atypical antipsychotics in the treatment of
schizophrenia: systematic overview and meta-regression analysis. BMJ 2000; 321(7273): 1371-1376
Giegling I, Balzarro B, Porcelli S, Schäfer M, Hartmann AM, Friedl M, Konte B, Krämer P, Möller HJ,
De Ronchi D, Stassen HH, Serretti A, Rujescu D: Influence of ANKK1 and DRD2 polymorphisms in response
to haloperidol. Eur Arch Psychiatry Clin Neurosci. 2013; 263(1): 65-74
Greil W, Zhang X, Stassen HH, Grohmann R, Bridler R, Hasler G, Toto S, Bleich S, Kasper S:
Cutaneous adverse drug reactions to psychotropic drugs and their risk factors - a case-control study.
Eur Neuropsychopharmacol. 2019; 29(1): 111-121
[get the article]
Greil W, de Bardeci M, Seifert J, Bernegger X, Cattapan K, Stassen HH, Wagner AL, Sieberer M,
Grohmann R, Toto S: Treatment of depression: Are psychotropic drugs appropriately dosed in women
and in the elderly? Dosages of psychotropic drugs by sex and age in routine clinical practice.
Hum Psychopharmacol. 2022; 37(1): e2809
[get the article]
Greil W, de Bardeci M, Müller-Oerlinghausen B, Nievergelt N, Stassen HH, Hasler G, Erfurth A,
Cattapan K, Rüther E, Seifert J, Toto S, Bleich S, Schoretsanitis G. Controversies regarding
lithium-associated weight gain: case-control study of real-world drug safety data.
Int J Bipolar Disord. 2023; 11(1): 34. doi: 10.1186/s40345-023-00313-8
[get the article]
Häfner H. Ist die Diagnose Schizophrenie noch sinnvoll? Psychiat Prax 2007; 34: 175-180
Kemp DE, Ganocy SJ, Brecher M, Carlson BX, Edwards S, Eudicone JM, Evoniuk G, Jansen W, Leon AC,
Minkwitz M, Pikalov A, Stassen HH, Szegedi A, Tohen M, Van Willigenburg AP, Calabrese JR:
Clinical value of early partial symptomatic improvement in the prediction of response and
remission during short-term treatment trials in 3369 subjects with bipolar I or II depression.
J Affect Disord. 2011; 130(1-2): 171-179
Khan A, Khan SR, Leventhal RM, Brown WA. Symptom reduction and suicide risk in patients
treated with placebo in antidepressant clinical trials: a replication analysis of the
Food and Drug Administration Database. Int J Neuropsychopharmacol 2001; 4(2): 113-118
Khan A, Khan SR, Leventhal RM, Brown WA. Symptom reduction and suicide risk among
patients treated with placebo in antipsychotic clinical trials: an analysis of the
food and drug administration database. Am J Psychiatry 2001; 158(9): 1449-1454
Laska EM, Meisner MJ. Nonparametric estimation and testing in a cure model. Biometrics 1992;
48(4): 1223-1234
Lett HS, Blumenthal JA, Babyak MA, Sherwood A, Strauman T, Robins C et al. Depression
as a risk factor for coronary artery disease: evidence, mechanisms, and treatment.
Psychosom Med 2004; 66(3): 305-315
Leucht S, Pitschel-Walz G, Abraham D, Kissling W. Efficacy and extrapyramidal side-effects of
the new antipsychotics olanzapine, quetiapine, risperidone, and sertindole compared to
conventional antipsychotics and placebo. A meta-analysis of randomized controlled trials.
Schizophr Res 1999; 35(1): 51-68
Leucht S, Busch R, Kissling W, Kane JM. Early prediction of antipsychotic nonresponse
among patients with schizophrenia. J Clin Psychiatry. 2007; 68(3): 352-360
Li M, Fletcher PJ, Kapur S. Time course of the antipsychotic effect and the
underlying behavioral mechanisms. Neuropsychopharmacology. 2007; 32(2): 263-272
Lötscher K, Anghelescu IG, Braun S, Bridler R, Stassen HH: Polypharmacy in psychiatry: clinical
practice versus empirical evidence. Eur Neuropsychopharmacol. 2010; 20 (Suppl. 3): 378-379
Mohr C, Braun S, Bridler R, Chmetz F, Delfino JP, Kluckner VJ, Lott P, Schrag Y, Seifritz E, Stassen HH:
Insufficient Coping Behavior under Chronic Stress and Vulnerability to Psychiatric Disorders.
Psychopathology 2014; 47: 235-243
Moragrega I, Bridler R, Mohr C, Possenti M, Rochat D, Sanchez Parramon J, Stassen HH:
Monitoring Mental Health and the Effects of Therapeutic Interventions through Self-Assessment
Voice Analyses. Res Psychother. 2021, 24(3): 250-262
[get the article]
Motivala SJ, Sarfatti A, Olmos L, Irwin MR. Inflammatory markers and sleep disturbance
in major depression. Psychosom Med. 2005; 67(2): 187-194
Papakostas GI, Perlis RH, Scalia MJ, Petersen TJ, Fava M. A meta-analysis of early
sustained response rates between antidepressants and placebo for the treatment of
major depressive disorder. J Clin Psychopharmacol 2006; 26(1): 56-60
Pollak TA, Lennox B, Müller S, Benros ME, Prüss H, Tebartz van Elst L, Klein H, Steiner J,
Frodl T, Bogerts B, Tian L, Groc L, Hasan A, Baune BT, Endres D, Haroon E, Yolken R,
Benedetti F, Halaris A, Meyer J, Stassen HH, Leboyer M, Fuchs D, Otto M, Brown DA, Vincent A,
Najjar S, Bechter K: An international consensus on an approach to the diagnosis and
management of psychosis of suspected autoimmune origin: the concept of autoimmune psychosis.
Lancet Psychiatry 2020; 7(1): 93-108
Posternak MA, Zimmerman M. Is there a delay in the antidepressant effect? A
meta-analysis. J Clin Psychiatry 2005; 66(2): 148-158
Rudisch B, Nemeroff CB. Epidemiology of comorbid coronary artery disease and
depression. Biol Psychiatry 2003; 54: 227-240
Skilton MR, Moulin P, Terra JL, Bonnet F. Associations between anxiety, depression,
and the metabolic syndrome. Biol Psychiatry. 2007; 62(11): 1251-1257
Stassen HH, Angst J, Hell D, Scharfetter C, Szegedi A. Is there a common resilience
mechanism underlying antidepressant drug response? Evidence from 2848 patients. J
Clin Psychiatry. 2007; 68(8): 1195-1205
Stassen HH, Anghelescu IG, Braun S, Hoffmann K, Rujescu D, Scharfetter C, Szegedi A, Tadic A:
Vulnerability to major psychiatric disorders, response to treatment and medical comorbidity —
shared genetic factors? Eur Neuropsychopharmacol. 2009; 19 (Suppl. 3): 262
Stassen HH, Anghelescu IG, Angst J, Böker H, Lötscher K, Rujescu D, Szegedi A, Scharfetter C:
Predicting Response to Psychopharmacological Treatment. Survey of Recent Results.
Pharmacopsychiatry 2011; 44: 263-272
Stassen HH, Delfino JP, Kluckner VJ, Lott P, Mohr C: Vulnerabilität und psychische Erkrankung.
Swiss Archives of Neurology and Psychiatry 2014; 165(5): 152-157
Stassen HH: Heterogeneity of schizophrenic disorders and link to chronically elevated IgM values.
Neurology, psychiatry and brain research 2018; 29: 23-24
Stassen HH, Bachmann S, Bridler R, Cattapan K, Herzig D, Schneeberger A, Seifritz E. Inflammatory
Processes linked to Major Depression and Schizophrenic Disorders and the Effects of Polypharmacy
in Psychiatry: Evidence from a longitudinal Study of 279 Patients under Therapy. Eur Arch
Psychiatry Clin Neurosci. 2021; 271(3): 507-520
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Herzig D, Schneeberger A, Seifritz E:
Detailing the Effects of Polypharmacy in Psychiatry: Longitudinal Study of 320 Patients
Hospitalized for Depression or Schizophrenia. Eur Arch Psychiatry Clin Neurosci. 2022;
272(4): 603-619
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Hartmann AM, Rujescu D, Seifritz E. Genetic
Predisposition to Unwanted Side Effects under Antidepressants and Antipsychotics: A
molecular-genetic study of 902 patients over 6 weeks. Eur Arch Psychiatry Clin Neurosci. 2025
2026; 276(2): 691-707. doi: 10.1007/s00406-025-02062-4. Epub 2025 Jul 28.
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Seifritz E. Polypharmacy in Psychiatry and
Weight Gain: Longitudinal Study of 832 Patients Hospitalized for Depression or Schizophrenia,
along with Data of 3,180 Students from Europe, the U.S., South America, and China.
Eur Arch Psychiatry Clin Neurosci. 2025; 275(4): 1001-1014. doi: 10.1007/s00406-024-01767-2.
Epub 2024 Mar 10.
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Hartmann AM, Rujescu D, Seifritz E, Weisbrod M,
Scharfetter C: Genetic Determinants of Antidepressant and Antipsychotic Drug Response:
A molecular-genetic study of 902 patients over 6 weeks. Eur Arch Psychiatry Clin Neurosci. 2025;
275(5): 1419-1435. doi: 10.1007/s00406-024-01918-5. Epub 2024 Oct 9.
[get the article]
Stassen HH, Bachmann S, Bridler R, Cattapan K, Hartmann AM, Rujescu D, Seifritz E, Weisbrod M,
Scharfetter C. Analysis of genetic diversity in patients with major psychiatric disorders
versus healthy controls: A molecular-genetic study of 1698 subjects genotyped for 100 candidate
genes (549 SNPs). Psychiatry Res. 2024; 333: 115720. doi: 10.1016/j.psychres.2024.115720
[get the article]
Szegedi A, Jansen WT, Van Willigenburg AP, Van der Meulen E, Stassen HH, Thase ME: Early
improvement as a predictor of treatment outcome in patients with major depressive disorder:
Why the first 2 weeks really matter —evidence from 6562 patients. J Clin Psychiatry 2009;
70(3): 344-353
Tamura RN, Faries DE, Feng J. Comparing time to onset of response in antidepressant clinical
trials using the cure model and the Cramer-von Mises test. Stat Med 2000; 19(16): 2169-2184
Thase ME. Comparing the methods used to compare antidepressants. Psychopharmacol Bull 2002; 36
Suppl 1: 1-17
Zhang M, Bridler R, Mohr C, Moragrega I, Sun N, Xu Z, Yang Z, Possenti M, Stassen HH:
Early Detection of the Risk of Developing Psychiatric Disorders: A Study of 461 Chinese University
Students under Chronic Stress. Psychopathology 2019; 52(6): 367-377
[get the article]
|
|
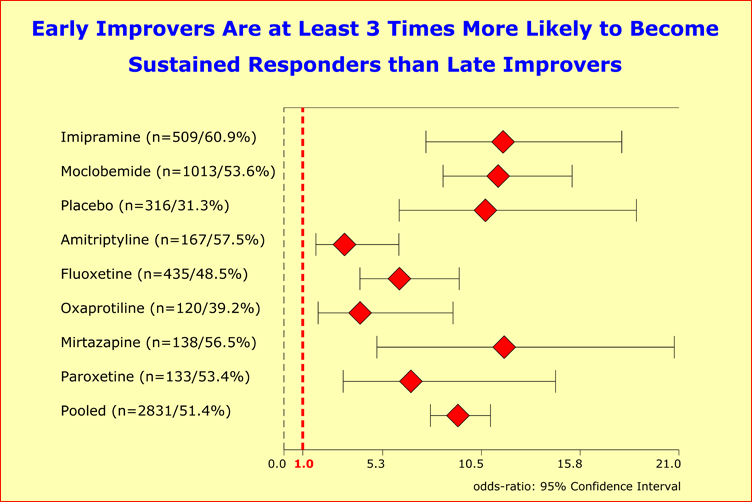
Sustained response is much more likely among early improvers independent of treatment modality as indicated by odds ratios that exceed 3 for all drugs and placebo. The estimates were derived by fitting a random-effects model which accounted for the between-study variation. The dotted line indicates an odds ratio of 1.
Please note: (1) patients showing no improvement throughout the first 2 weeks of
treatment have a probability of <15% to later become responders; (2) this probability drops below 8%
after 3 weeks without improvement.
|
|
| [ Mail to Webmaster ] k454910@ifrg.ch |